WCN Diverse Nurse Faculty Mentorship Program
October 11, 2023
No Comments
WCN’s mission is to support a healthy Washington by engaging nurses’ expertise, influence, and perspective and by building a diverse, highly qualified nurse workforce to meet future demands. When WCN surveyed nurse faculty in 2017, we found
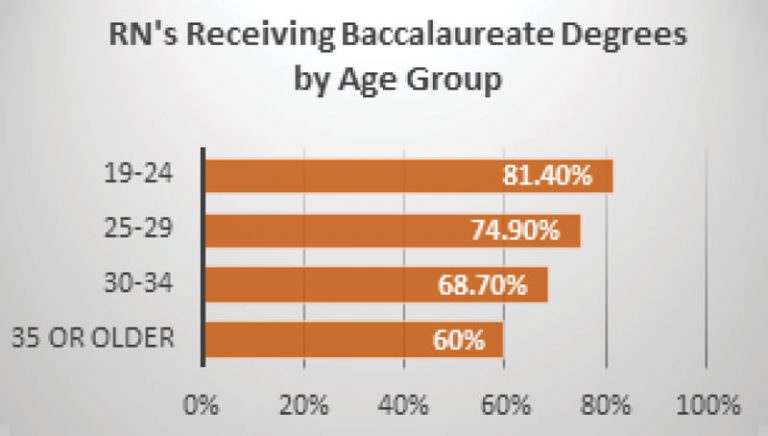
that approximately 40% of nurse faculty planned to retire by 2027, and that the racial and ethnic diversity of nurse faculty is less than the nursing student population and the population of the state of Washington
As a result of the COVID-19 pandemic, retirement and turn-over among nurse faculty appears to have accelerated. In addition, the pandemic has highlighted persistent disparities in care. For example, Black/African American rates of COVID-19 are twice the white population and Hispanic or Latinx rates of COVID-19 are three times the rate of the white population. In addition, there was harmful bias against Asians due to negative associations between COVID-19 and China.
Previous
Next

HOW TO APPLY
Click on the link below to fill out and submit a mentor or mentee application.
(Application should take an estimated 15-20 minutes to complete.)
Mentor application link: https://www.surveymonkey.com/r/CLXDTQF
Mentee application link: https://www.surveymonkey.com/r/C8PZTQB
The deadline for applications EXTENDED to Mon, Dec 18, 2023 (11:59 p.m.), Sun, Dec 3, 2023.
Additional Information
Once submitted, the selection committee will review applications pairing mentors and mentees to participate in the program. Efforts will be made to match mentees with the type of mentor they believe would benefit them most. Selected participants will be notified the week of December 18.
Questions? Email, info@wcnursing.org